Definition
The strict definition of transposition physiology is that the oxyhemoglobin saturation of blood in the pulmonary artery is higher than that in the aorta. This makes the circulation inefficient since pulmonary blood flow is already oxygenated (i.e. ‘effective’ pulmonary blood flow is low). The prototypical patient with transposition physiology is one with dTGA±VSD, though it can occur in other anatomies in which the atria and ventricles are septated enough to prevent complete mixing and there is atrioventricular or ventriculoarterial discordance.
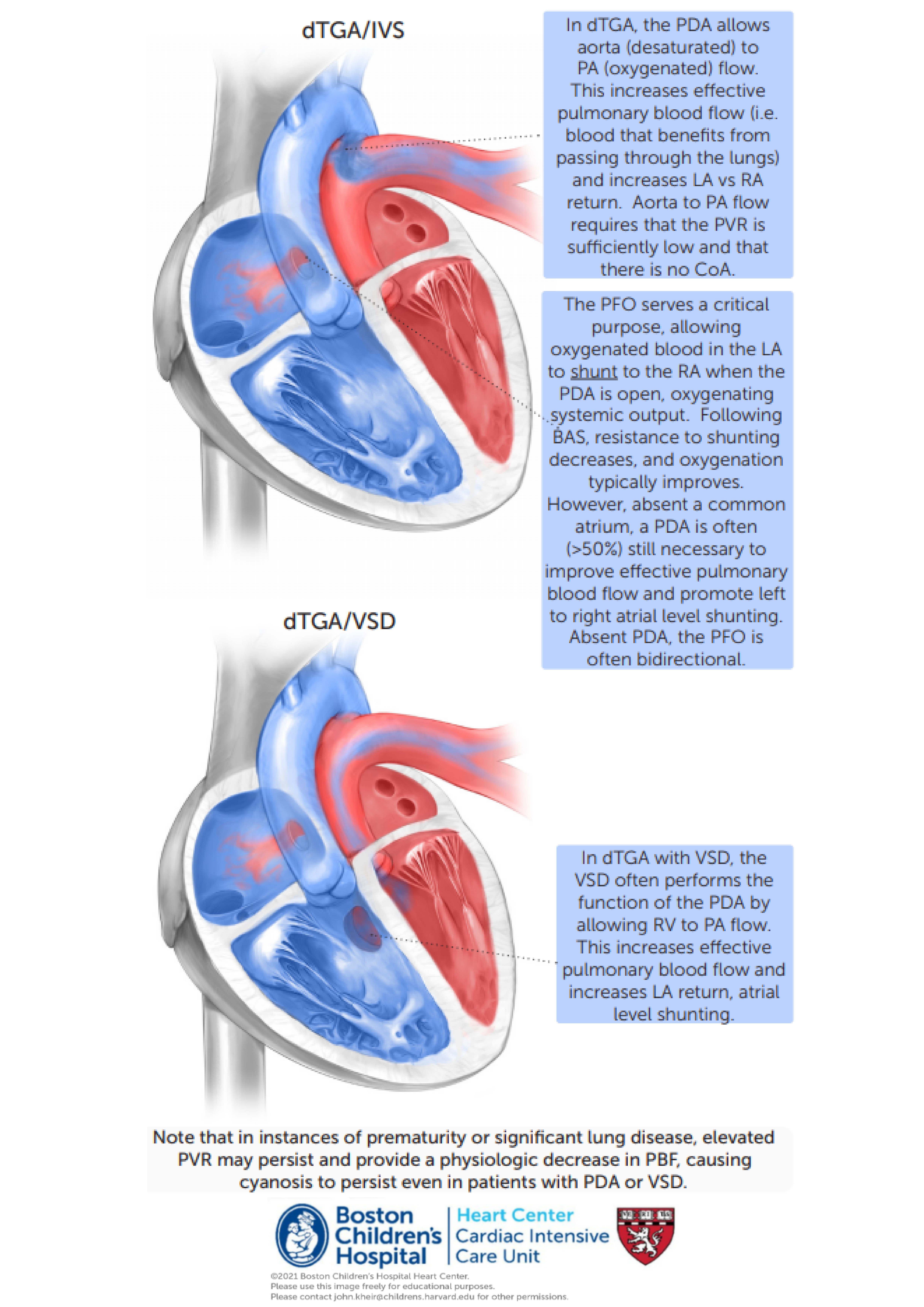
Treatment considerations Maintaining systemic oxygenation requires two things. (1) The shunting of oxygenated blood from the pulmonary circulation into the systemic circulation. This primarily occurs at the atrial level. (2) Maintaining ‘effective’ pulmonary blood flow by sending deoxygenated blood to the pulmonary arteries. These two phenomena are anatomically linked, as increasing effective pulmonary blood flow increases LA return > RA return and drives atrial level shunting. Thus, the status of the atrial septum is paramount.
- In the most extreme cases, the atrial septum is nearly intact (including no sprung PFO), resulting in immediately life-threatening hypoxemia (saturations <50%). In such patients, emergent septostomy is indicated. (When a PFO is not present, the procedure itself is technically more complex since a defect must be created.) Additionally, volume administration may ‘spring’ open (i.e. stretch) the PFO, and ventilation with paralysis may diminish VO2 and stabilize the patient. Treatment with 100% oxygen may lower PVR and increase dissolved oxygen in LA return, both of which may improve systemic saturations. iNO may be useful in patients thought to have elevated PVR. In instances where BAS is not immediately possible, hypothermia and ECMO support may be life saving. PGE should be administered to maintain ductal patency.
- More typically, the newborn will exhibit an acceptable degree of atrial level shunting in the presence of a PDA or VSD. Indications for BAS may include significant cyanosis (saturations <60%) or signs of LA hypertension. The supportive maneuvers above are sometimes required and are often considered indications for BAS. (In intubated patients, always r/o pulmonary vein desaturation due to reversible causes such as ETT malposition.)
- Even in patients with a sizeable atrial level defect, maintaining ductal patency using PGE1 is sometimes necessary, emphasizing that blood in the atrium is usually shunting rather than mixing, and therefore LA return (i.e. Qp) must exceed RA return (i.e. Qs) in order to shunt. The LA saturation in dTGA usually approaches 100%.
- In any patient, atrial level shunting may be diminished by hypovolemia, and oxygen saturations may be responsive to volume. •Most patients with VSD are sufficiently oxygenated without PGE due to RV to PA flow which increases LA return in a similar way to PDA flow.